The 2026 Front Desk Solution: How a Bilingual AI Receptionist Transforms Practice Workflow and Recovers Revenue
-

Judah is the Marketing Lead at Medical Office Force. He specializes in new technology growth and on practical insights that help clinics succeed in a rapidly changing healthcare landscape.
The modern medical front desk is under immense pressure, with staff juggling high call volumes and endless administrative tasks. At the Medical Office Force (MOF), we understand that answering the telephone is an essential part of providing the care your patients expect and deserve.
As of March 31, 2026, bilingual AI medical front-desk reception in the U.S. looks real, early, and economically promising. While public data still does not give a clean national adoption rate for the exact niche of a “bilingual AI medical front-desk receptionist,” what we do have is strong adjacent evidence: over 80% of physicians say they now use AI professionally, 71% of hospitals reported using predictive AI in 2024, and the fastest-growing hospital AI uses included scheduling and billing. In a February 2026 MGMA poll, practice leaders using AI/automation for access most often named scheduling (31%) and calls (27%).
The Bilingual Imperative and Patient Flow
The bilingual piece matters immensely because the U.S. patient base is highly multilingual. Census data reports that 22% of people age 5 and older speak a language other than English at home, and KFF estimates about 26 million people in the U.S. have limited English proficiency (LEP), with Spanish accounting for 62% of adults with LEP. Furthermore, the Department of Health and Human Services (HHS) mandates that covered entities have language-assistance obligations, and the Section 1557 rule requires “reasonable steps” to provide meaningful access for people with LEP.
To meet this need, Medical Office Force provides an AI virtual receptionist that answers calls instantly and seamlessly switches between English and Spanish. Our technology provides an accurate response with less than 100 milliseconds of latency to language changes. 1 This lightning-fast, zero-hold-time interaction ensures patients feel heard and respected in their preferred language without the frustrating delays typical of older automated systems.
Outcomes: Experience, Access, and Engagement
On outcomes, the evidence is strongest for three things:
- Better language support improves experience and access: Systematic reviews show that language-concordant care improves outcomes in the majority of studies, and professional interpreters improve comprehension, satisfaction, and delivery of care for patients with LEP.
- Reminder/outreach workflows work: A systematic review found reminders reduced non-attendance by a weighted mean of 34% relative to baseline, with manual phone calls outperforming automated reminders (39% vs 29% relative reduction).
- Targeted outreach works: A randomized safety-net primary-care initiative found that adding targeted live telephone outreach to automated reminders reduced no-show rates from 36.2% to 32.8% overall.
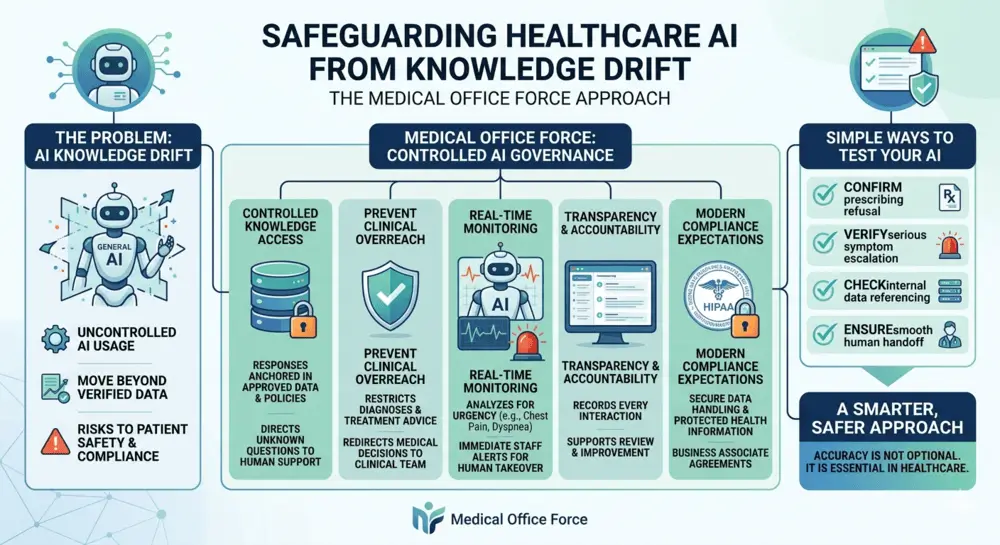
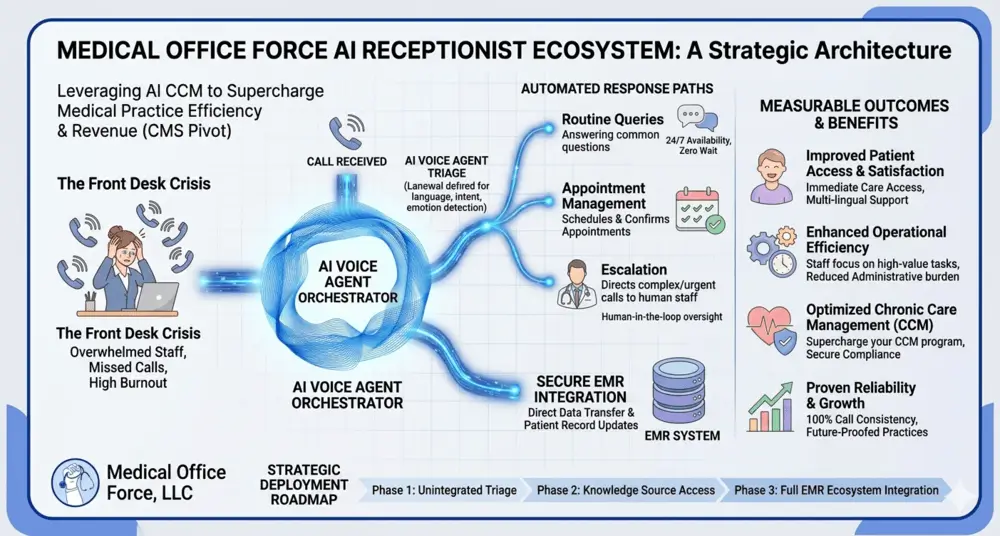
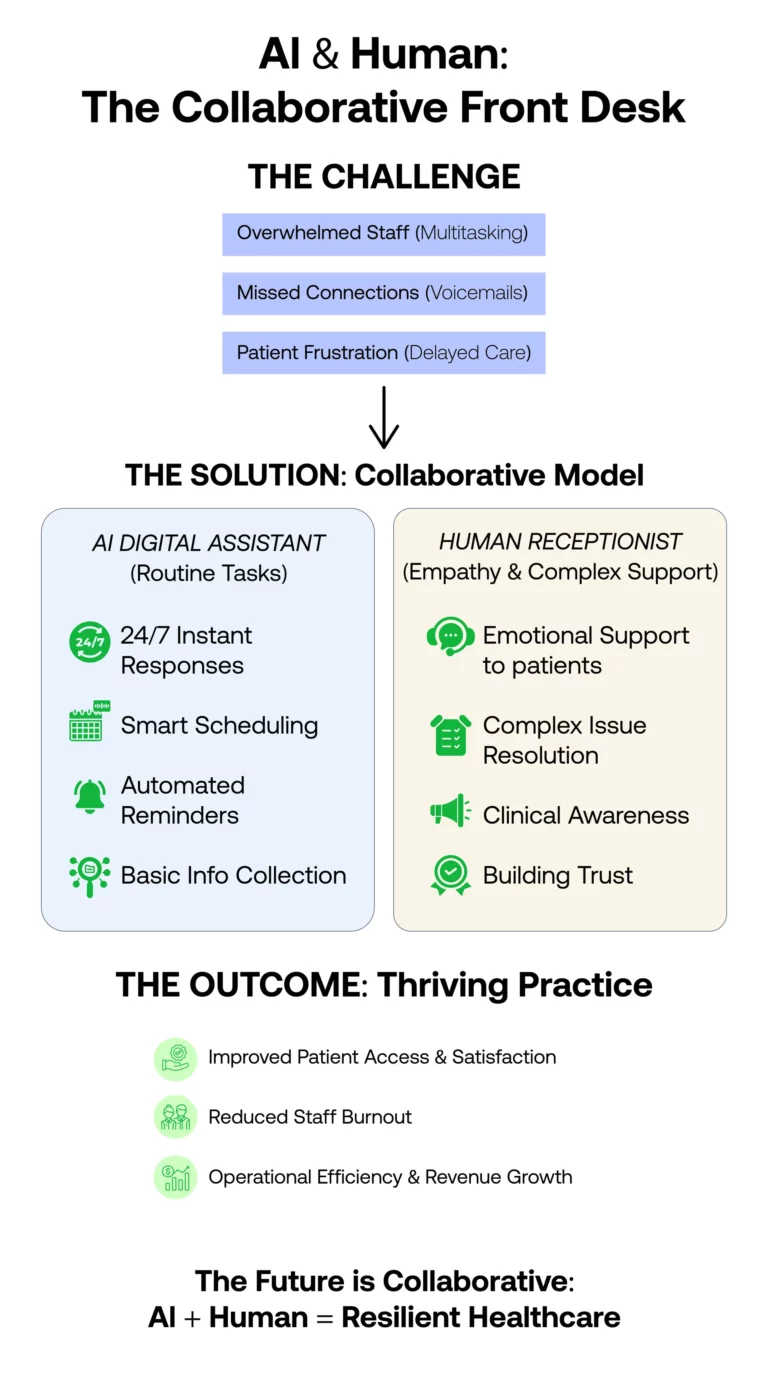
For bilingual front-desk AI specifically, that means the best 2026 model is hybrid, not fully autonomous. At MOF, we recommend using AI for first-pass tasks such as language selection, scheduling, reminders, directions, registration, simple billing questions, and after-hours capture; then escalating failed contacts, symptom calls, consent discussions, and complex issues to your staff or a qualified professional interpreter. That approach fits both the evidence and the compliance environment, because AHRQ notes a high risk of error when LEP patients are handled without qualified professional interpretation.
The ROI Case and Telehealth Equity
The ROI case is strongest when the system does three jobs well:
- Recovers missed calls and after-hours demand into booked visits: Healthcare clinics can lose an average of 74.1% of inbound calls to voicemails or hangups during peak hours and lunch breaks. Furthermore, data reveals that 34.8% of after-hours callers express active intent to book appointments or purchase services. By ensuring every call is answered seamlessly, practices plug massive revenue leaks. For example, capturing just 20 missed calls a day that result in two retained patients (valued at $200 per patient) recovers approximately $96,000 annually. Real-world deployments of bilingual AI agents across clinic networks have successfully captured thousands of after-hours appointments, recovering upwards of $180,000 in annual revenue and achieving a 15x ROI in just six months.
- Reduces no-shows with bilingual reminders and smart escalation: Automated, language-concordant outreach ensures LEP patients understand their appointment details, directly lowering missed appointment rates and preserving schedule density.
- Redeploys front-desk labor from repetitive calls to higher-value work: An AI receptionist operates flawlessly 168 hours a week and possesses the concurrent call capacity of 2 to 2.5 full-time staff members. By offloading routine scheduling to AI, practices dramatically lower staff burnout, reduce turnover costs, and allow human talent to focus on complex, in-clinic patient care.
That is why English-Spanish usually gives the fastest return, and why the next language should be chosen from your own call logs rather than guesswork. A conservative labor-only view already shows meaningful value. The BLS reports median 2024 pay for medical secretaries and administrative assistants at $44,640. So even 0.25 FTE of front-desk capacity redeployed is worth about $11,160/year in direct wages, and 0.5 FTE is about $22,320/year, before benefits and overhead. If the same system also reduces no-shows or captures even a small number of otherwise-lost appointments, total ROI can turn positive quickly.
There is also an equity and telehealth ROI. A 2025 systematic review found LEP patients were often less likely to use telemedicine, and across all seven modality studies, they had lower video use than English-proficient patients. Bilingual front-end support is not just a courtesy; it removes one of the first barriers to virtual care, access, and follow-up.
The Bottom Line for 2026
Bilingual AI front-desk reception is moving from pilot to operations, especially for English-Spanish workflows. The best-proven benefits are improved access, better no-show performance when paired with live follow-up, staff relief, and better service for LEP patients. The best business case is not “replace the front desk,” but “augment the front desk, recover demand, and escalate intelligently.”
Medical Office Force: 2026 ROI Brief & Pro Forma
Medical practices receive an average of 53 calls per provider per day, and the industry average shows that up to 24% of inbound calls are abandoned or go to voicemail. Furthermore, each provider generates approximately 66 minutes of phone call overhead daily. By augmenting your staff with MOF’s bilingual AI receptionist, you can recover this lost time and revenue data automation..
| Metric | 1-Provider Practice | 5-Provider Practice | 20-Provider Practice |
|---|---|---|---|
| Average Daily Call Volume | 53 calls | 265 calls | 1,060 calls |
| Estimated Abandoned/Missed Calls (24%) | 12 calls/day | 63 calls/day | 254 calls/day |
| Staff Time Recovered Daily | ~1.1 hours | ~5.5 hours | ~22 hours |
| Minimum FTE Redeployed | 0.25 FTE | 1.0 FTE | 4.0 FTE |
| Annual Baseline Labor Savings (at BLS $44,640) | $11,160 | $44,640 | $178,560 |
(Note: Total ROI scales significantly higher when factoring in the actual revenue from capturing missed appointments, reducing no-shows, and eliminating after-hours leakage).
5 Questions Practice Owners Should Ask Before Implementing a Bilingual AI Receptionist
- How much revenue and patient trust are you currently losing due to the industry average of 24% of inbound calls going to voicemail or being abandoned on hold?
- Does the AI platform use a hybrid model? Is it capable of handling first-pass administrative tasks while intelligently escalating complex clinical or emotional issues to your human staff to remain compliant?
- What is the latency of the voice agent? Can the system detect a language change and respond in Spanish in under 100 milliseconds to preserve the natural flow of conversation and keep patients from hanging up? 1
- Does the AI natively integrate with your Electronic Health Record (EHR)? Will the AI seamlessly read and write scheduling data to Epic, Cerner, AthenaHealth, or your specific practice management software?
- How does the system support your Section 1557 compliance? Does the AI accurately handle Spanish dialects and LEP patient interactions equitably without relying on easily confused, basic translation algorithms?
FAQs About Bilingual AI Receptionists and ROI
- Will this AI voice agent completely replace my front desk staff?
No. Our AI voice agent is designed to augment your team, not replace them. It removes repetitive calls (like simple scheduling and FAQs) so your human team can focus on complex patient care, in-clinic experiences, and higher-value administrative work.
- How fast does the AI switch languages if a caller starts speaking Spanish?
The Medical Office Force AI features instantaneous language detection. It transitions from English to Spanish with less than 100 milliseconds of latency, creating a natural, conversational experience without forcing patients to navigate a “Press 2 for Spanish” menu. 1
- What is the real return on investment (ROI)?
ROI comes from three areas: recovering missed calls, reducing no-shows, and redeploying staff. By simply saving 0.5 FTE of front-desk capacity, a practice saves over $22,000 annually in direct wages. When you add the captured revenue from patients who would have otherwise hung up and called a competitor, the system pays for itself rapidly.
- How does a bilingual AI help with our Section 1557 compliance?
Under the Affordable Care Act’s Section 1557, medical practices must take reasonable steps to provide meaningful access to LEP patients. Providing a highly accurate, culturally competent Spanish AI front desk removes immediate language barriers, improving access to virtual care, appointment booking, and basic triage.
- How does the hybrid model actually work in practice?
The AI acts as the first line of defense. It handles language selection, books appointments, provides directions, and answers basic billing questions. If a patient describes a medical symptom, requests a complex procedure, or simply gets frustrated, the AI instantly escalates the call to your staff, ensuring patient safety and trust.
- Can the AI handle calls after hours?
Yes. The MOF AI operates 24/7/365. This allows your practice to capture high-intent patients who call during the evening or on weekends, ensuring their appointments are booked directly into your calendar before they can call another clinic.
- How long does it take to implement this in my clinic?
Implementation is remarkably fast. MOF’s system can be activated within days without requiring heavy, disruptive technical integration and syncs securely with major practice management software like Panacea, Epic, Cerner, and AthenaHealth.
References & Supporting Data
- #1. American Medical Association (AMA): 2026 Physician AI Survey, detailing that over 80% of physicians now use AI professionally, with scheduling and calls acting as primary adoption drivers. 2
- #2. U.S. Census Bureau & KFF: Demographic studies showing 22% of individuals age 5+ speak a language other than English at home, and approximately 26 million U.S. residents have limited English proficiency (LEP), with Spanish making up 62% of that demographic. 3
- #3. U.S. Department of Health and Human Services (HHS): Section 1557 of the Affordable Care Act final rule, mandating meaningful language access and establishing strict non-discrimination protections for LEP individuals interacting with Patient Care Decision Support Tools (PCDSTs) and AI. 4
- #4. Bureau of Labor Statistics (BLS): 2024 median wage data reporting medical secretaries and administrative assistants earn $44,640 annually.
- #5. Industry Call Center Analytics: Operational benchmarks demonstrating that 24% of inbound medical calls are missed or abandoned, up to 74.1% are lost during peak times, and 34.8% of after-hours callers show high booking intent. 5
- #6. Voice AI Performance Benchmarks: Enterprise AI latency tracking demonstrating that top-tier systems achieve sub-100 millisecond response times, enabling imperceptible code-switching between English and Spanish. 1
Works cited
- Spanish and Translate: Transync AI’s Real-Time Solution for 2026, accessed March 31, 2026, https://www.transyncai.com/blog/spanish-and-translate-transync-ai-solution/
- 2026 Physician Survey on Augmented Intelligence – American Medical Association, accessed March 31, 2026, https://www.ama-assn.org/system/files/physician-ai-sentiment-report.pdf
- Hispanic Americans’ experiences with health care | Pew Research Center, accessed March 31, 2026, https://www.pewresearch.org/science/2022/06/14/hispanic-americans-experiences-with-health-care/
- HHS Recent Guidance on AI Use in Health Care | ReedSmith, accessed March 31, 2026, https://www.reedsmith.com/our-insights/blogs/health-industry-washington-watch/102k29k/hhs-recent-guidance-on-ai-use-in-health-care
- 37 AI Receptionist Statistics 2026 [347K Calls Analyzed] – NextPhone, accessed March 31, 2026, https://www.getnextphone.com/blog/ai-receptionist-statistics