Why Small Clinics Must Prepare for the CMS ACCESS Model in 2026
-

Medical Director, Medical Office Force LLC | Athens, Georgia
Alumnus: SMS Medical College, Emory University, University of Alabama at Birmingham
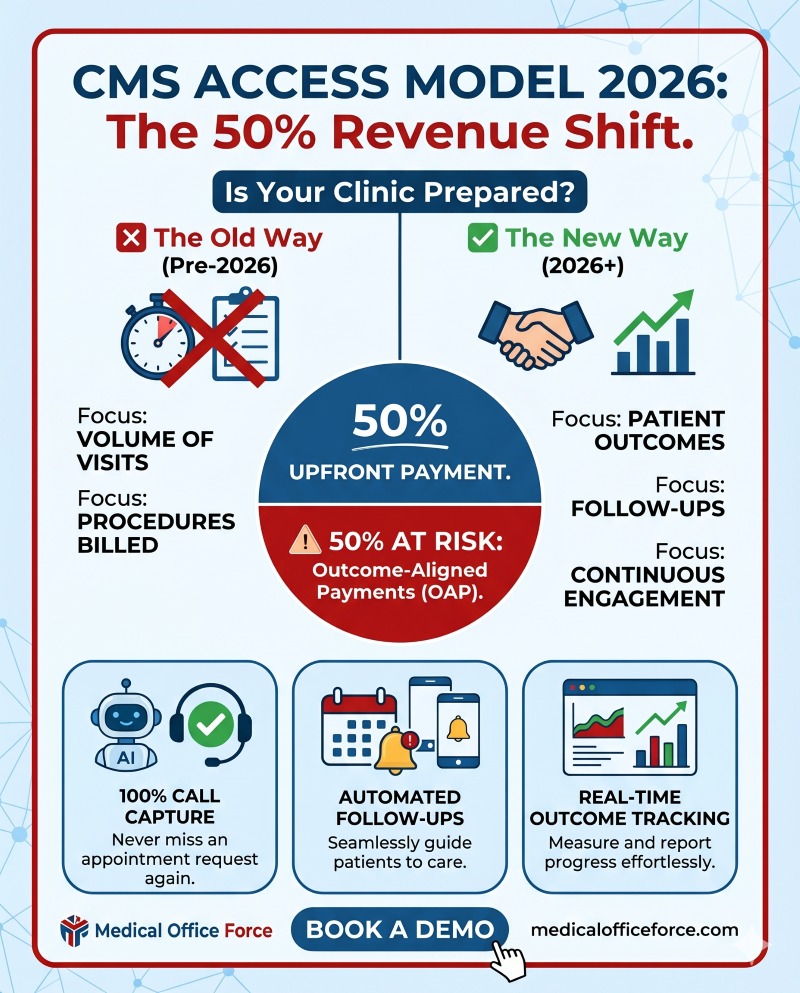
The 50% Revenue Risk Small Practices Can’t Afford to Ignore
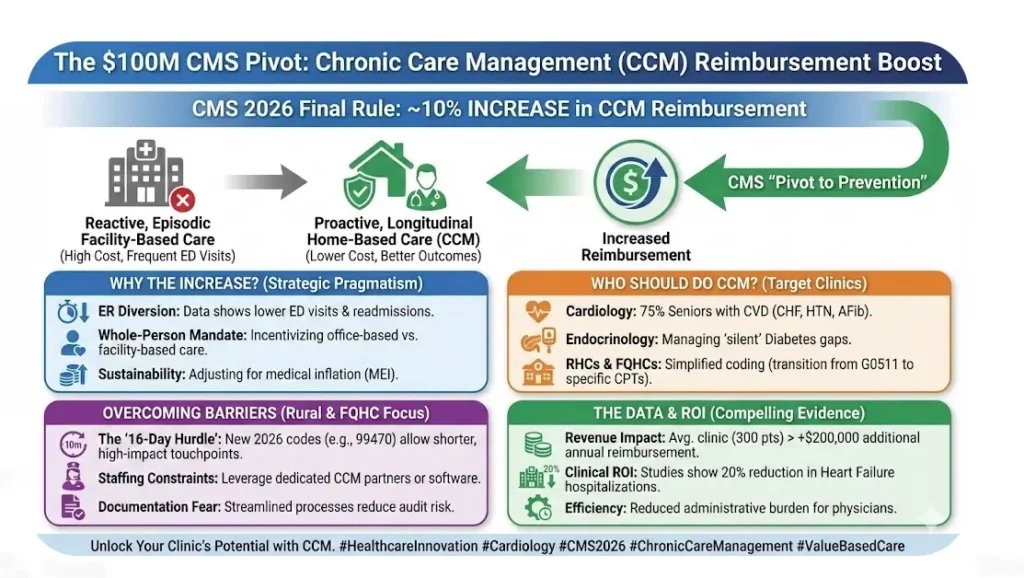
The healthcare payment landscape is shifting from “volume” to “value.” With the introduction of the CMS ACCESS Model in 2026, small clinics are no longer just competing on patient care – they are being evaluated on Outcome-Aligned Payments (OAP).
For independent practices, this shift is the difference between financial stability and a 50% revenue loss.
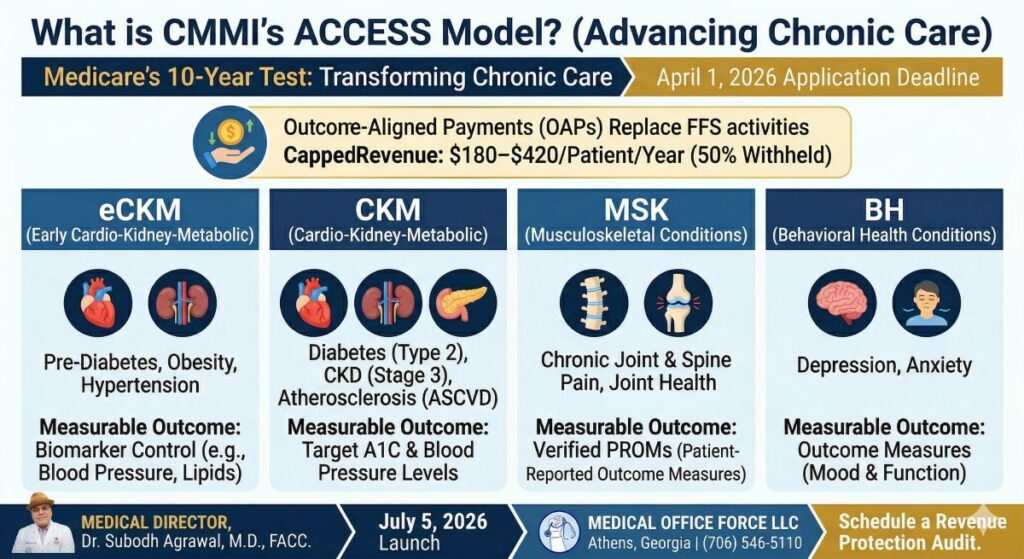
What is the CMS ACCESS Model?
The CMS ACCESS Model is a new value-based care initiative that introduces Outcome-Aligned Payments (OAP). Under this model, up to 50% of clinic revenue is tied directly to measurable patient outcomes, engagement levels, and efficiency metrics.
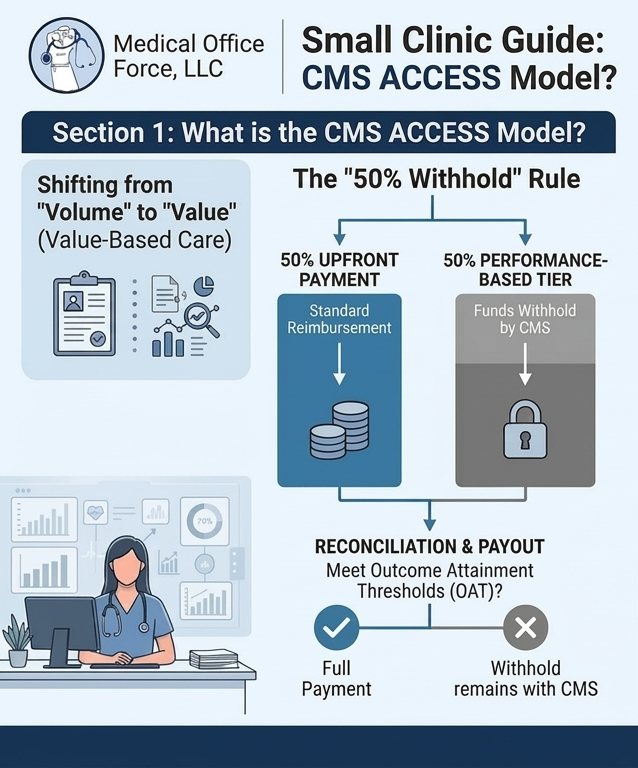
The “50% Withhold” Rule Explained
[See how these tiers compare to traditional FFS reimbursement models.]
50% Upfront Payment: Standard reimbursement for services rendered.
- 50% Performance-Based Tier: Funds held back by CMS and released only if the clinic meets specific Outcome Attainment Thresholds (OAT).
Key Challenges for Small Clinics in 2026
Large hospital systems have the overhead to manage complex reporting. Small clinics, however, face three critical “Risk Factors”:
- Staffing Constraints: Limited front-desk support leads to missed calls and delayed follow-ups.
- Manual Workflows: Reliance on paper or manual data entry results in missed reporting deadlines and inaccurate SST (Substitute Spend Adjustment) tracking.
- Patient Leakage: When patients seek care outside your network due to slow response times, your clinical control and revenue both drop.
Why Patient Engagement is the Primary Revenue Driver
How Automation Protects Your Bottom Line
To compete with larger systems, small clinics must adopt AI-driven healthcare automation. This is no longer a luxury; it is a compliance necessity.-
-
- AI Call Handling: Ensures 100% of patient inquiries are captured.
- Automated Reminders: Reduces no-shows and improves OAT scores.
- Integrated Reporting: Syncs clinical outcomes with CMS requirements automatically.
-
Action Plan: Preparing Your Clinic for the ACCESS Model
- Audit Your Communication: Identify your “Missed Call Rate.” Every missed call is a threat to your OAP.
- Digitize Patient Follow-ups: Implement automated systems to track care continuity.
- Monitor OAT Monthly: Do not wait for year-end reports. Use real-time dashboards to track performance.
- Eliminate Care Leakage: Use tech-enabled engagement to keep patients within your practice ecosystem.
The Opportunity: Agility Over Scale
Conclusion: Adapt or Fall Behind
The CMS ACCESS Model is a fundamental shift in healthcare economics. By investing in patient engagement and AI-driven automation today, your clinic can secure its financial future and outperform the competition.Frequently Asked Questions (FAQ)
How does the CMS ACCESS Model affect small clinic revenue?
It places up to 50% of total revenue at risk. This “withhold” is only paid out if the clinic meets specific patient outcome and engagement targets.
What is Outcome-Aligned Payment (OAP)?
OAP is a payment structure where a significant portion of reimbursement is tied to the quality of care and patient health results rather than the number of visits.
How can AI help clinics with the ACCESS Model?
AI handles high-volume tasks like patient scheduling, follow-up reminders, and data tracking, ensuring the clinic hits the engagement metrics required to trigger full payment.
Optimize Your Revenue with Medical Office Force
Stop losing revenue to missed calls and manual processes. Medical Office Force specializes in helping small clinics navigate the CMS ACCESS Model.
- Zero Missed Calls
- Automated Patient Engagement
- Reduced Care Leakage