The $144,000 Silent Leak: How Missed Calls Are Draining Your Medical Practice
In a busy medical practice, the phone never really stops ringing. It rings during clinic hours, over lunch, and even after the last patient has left.
Each call represents something important. A new patient trying to book an appointment. An existing patient concerned about symptoms. A referral from another physician.
But what happens when that call goes unanswered?
For many practices, a missed call feels like a minor operational issue. In reality, it is a silent revenue leak. Over time, these missed opportunities can cost a practice thousands of dollars every month without leadership fully realizing it.
The Real Cost of a Missed Call
Healthcare is deeply personal, but it is also highly competitive. When a patient cannot reach your practice, they rarely wait. Most will simply call another provider.
Even a small number of missed calls can have a measurable financial impact.
Consider a conservative example:
10 missed calls per day
40 percent of those are appointment related
4 lost appointments per day
Average visit value: 150 dollars
This results in 600 dollars lost per day, 12,000 dollars lost per month, and 144,000 dollars lost per year.
This calculation only reflects immediate visit revenue. It does not account for follow up care, procedures, or long term patient value.
Why Patients Do Not Call Back
When patients call a medical practice, they are often anxious or in discomfort. They are looking for reassurance and timely access to care.
If the call is not answered, that moment of trust is disrupted. Most patients do not leave a voicemail or wait for a callback. They move on to the next available provider.
This is not just a missed interaction. It is a lost opportunity to build a patient relationship.
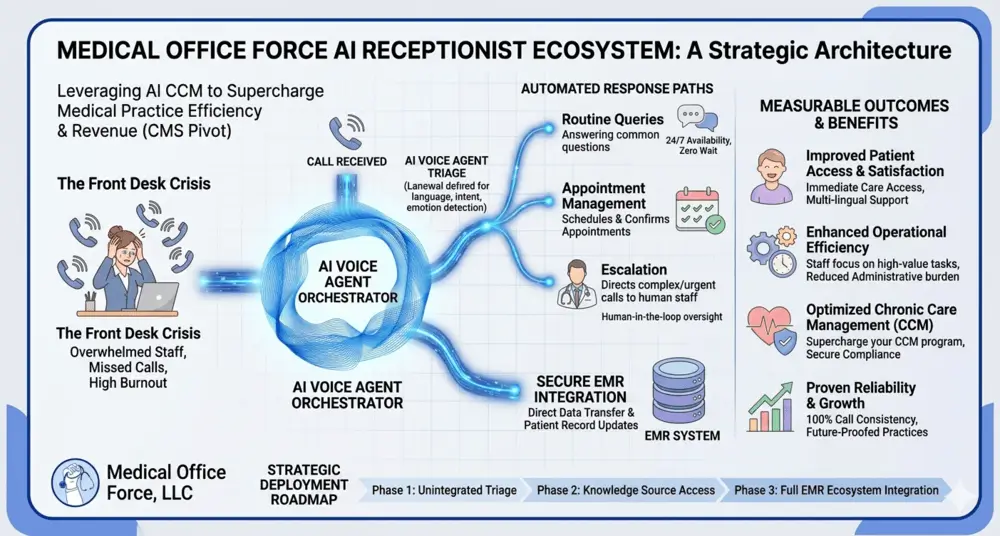
The Reality at the Front Desk
Missed calls are rarely the result of negligence. They are usually the result of capacity limitations.
Front desk teams are responsible for multiple critical tasks at the same time. Patient check ins and check outs, insurance verification, payment collection, and in person coordination all compete for attention.
During peak hours, handling phone calls becomes increasingly difficult. Calls may be placed on hold, rushed, or missed entirely.
Over time, this affects both operational efficiency and patient experience.
The Hidden Impact on Reputation and Growth
The consequences of missed calls extend beyond immediate revenue loss.
A poor phone experience often leads to negative online reviews. Patients today actively evaluate practices based on responsiveness and ease of communication.
Missed calls can also disrupt referral relationships. If referring providers cannot reliably reach your practice, they may begin directing patients elsewhere.
Growth in healthcare depends not only on clinical excellence but also on accessibility.
Why This Problem Often Goes Unnoticed
One of the biggest challenges is lack of visibility.
Many practices do not track total incoming calls, call abandonment rates, hold times, or conversion from calls to appointments.
Without this data, it is easy to underestimate the scale of the problem.
A simple question can reveal the gap. How many calls did we miss last week?
If the answer is unclear, there is likely a missed opportunity to improve both performance and revenue.
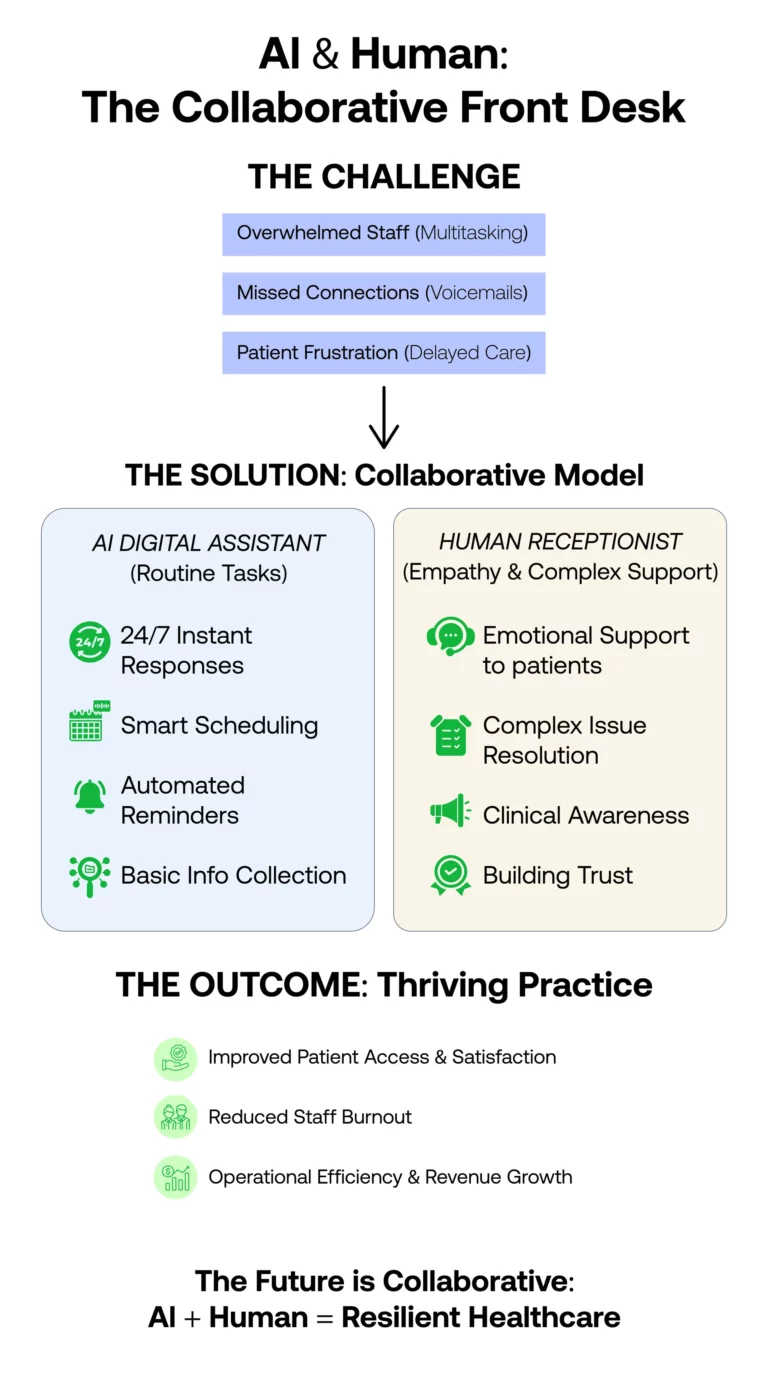
The Solution: Strengthening Systems, Not Increasing Pressure
The answer is not to push staff harder. Most teams are already working at capacity.
The solution lies in improving systems and support. This may include structured call workflows, extended coverage, dedicated call handling support, and real time tracking.
Practices that implement these changes often see immediate improvements in both patient satisfaction and financial performance.
Conclusion
Every phone call represents a patient seeking care.
When that call is missed, the impact goes beyond a single appointment. It affects revenue, reputation, and long term growth.
By improving communication systems and reducing missed opportunities, practices can retain more patients and build a stronger, more sustainable future.
Frequently Asked Questions
How much revenue can a medical practice lose from missed calls?
Even a small number of missed calls can lead to significant losses. Missing just four appointment related calls per day can result in around twelve thousand dollars in lost monthly revenue. Over a year, this can exceed one hundred thousand dollars depending on the practice size.
Why do patients not call back if their first call is missed?
Most patients expect quick access to care. If a call is not answered, they often assume the practice is unavailable and immediately contact another provider.
What is call abandonment rate in a medical practice?
Call abandonment rate refers to the percentage of callers who hang up before reaching a staff member. A high rate usually indicates long hold times or insufficient call handling capacity.
How can medical practices reduce missed calls?
Practices can improve call handling by strengthening systems, extending coverage, and using structured workflows. Many also benefit from additional call support or automation for routine queries.
Do missed calls affect patient reviews and reputation?
Yes. Poor phone experience is a common reason for negative reviews. Difficulty in reaching a practice reduces trust and impacts patient decisions.
What is the best way to track missed calls in a clinic?
The most effective way is to use call tracking systems that monitor incoming calls, missed calls, hold times, and conversion rates. This helps identify gaps and improve performance.