Q1: What is the main disadvantage of a physician practice and a home health agency using separate, disconnected EMR systems for Texas Medicaid telemonitoring?
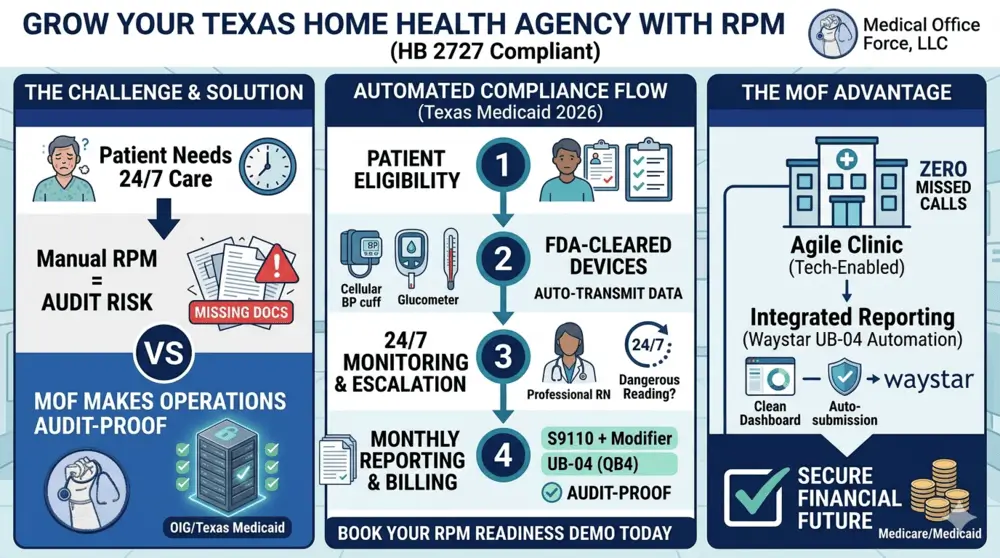
Operating on disconnected EMRs creates clinical and operational “silos,” forcing staff to manually toggle between multiple portals to log biometric readings, update patient progress, and coordinate care . This fragmentation leads to major inefficiencies, data entry errors, and a high risk of “note bloat” or information overload . Most critically, under Texas H.B. 2727, HHAs are legally mandated to share their established care plans and ongoing physiological outcome measures with the patient’s prescribing physician. When systems are siloed, agencies must resort to manual faxes or emails, which slows clinical workflows and creates significant HIPAA compliance risks .
Q2: What are the main clinical and administrative advantages of using a single, unified EMR platform to manage both physician and home health telemonitoring?
A unified, integrated EMR platform builds a secure digital bridge that connects patients, HHAs, and physicians in a single, shared workspace . For the clinical team, vital signs flow automatically from FDA-cleared medical devices directly into the patient’s chart, completely eliminating double data entry and reducing staff administrative time by over 30%. Bi-directional integration ensures that when a home health nurse updates a care plan, it immediately populates within the physician’s native EHR (such as Epic, athenahealth, or eClinicalWorks), enabling immediate, data-informed clinical decisions during virtual or in-office encounters.
Q3: How can a busy physician practice participate in a Medicaid telemonitoring program if they lack the staff or time to run it internally?
A busy practice should delegate the “heavy lifting” by partnering with a licensed home health agency or contracting a specialized, full-service RPM/CCM vendor . These partners act as a direct clinical extension of the physician’s practice under general supervision . They handle patient outreach, clinical onboarding, and local device delivery, and provide a 24/7 Health Operations Center (HOC) staffed with licensed clinical teams to monitor incoming biometric readings . This allows the physician to focus entirely on high-level medical decision-making while comfortably billing for digital care management services.
Q4: How do home health agencies or third-party vendors help physicians identify and “scrub” eligible high-risk Medicaid patients?
The EMR vendor or HHA partner can utilize advanced population health analytics to scan the physician’s active patient panel. The software automatically filters and “scrubs” patient demographics to identify adults with Texas Medicaid or STAR+PLUS plans who are diagnosed with diabetes, hypertension, or both. It then identifies eligible high-risk candidates by cross-referencing their clinical charts for at least one state-mandated risk factor, such as two or more hospitalizations in the prior 12 months, frequent emergency department visits, a documented history of falls, or poor medication adherence.
Q5: How can a vendor or HHA manage the prior authorization process for the TMHP Form F00032?
The HHA partner or software vendor handles the entire administrative process of securing prior authorizations. They leverage the integrated EMR to auto-populate the revised Texas Medicaid “Home Telemonitoring Services Prior Authorization Request” (Form F00032) with necessary NPIs, taxonomy codes, and documented clinical risk factors. They then submit the completed Form F00032 directly via the electronic prior authorization portal on the TMHP website. Additionally, the software tracks the approved authorization periods (which are valid for up to 90 days or 180 days under STAR+PLUS MCOs) and automatically alerts staff to initiate renewals before the current period expires.
Q6: Can a third-party vendor or HHA compliantly call patients for CCM, RPM, and BHI under physician supervision?
Clinical staff employed by the vendor’s Health Operations Center (HOC) or the home health agency conduct all patient-facing calls and clinical triaging . Because Medicare and Medicaid permit these digital care services under general supervision, the clinical staff does not need to be in the same physical building as the physician . The partner’s clinical team calls the patient to perform medication reconciliations, review care plans, and integrate mental health checks. All call durations, patient comments, and clinical assessments are automatically recorded, timestamped, and uploaded directly to the patient’s EHR chart, providing the exact documentation the physician needs to compliantly bill for monthly management time .
Q7: How does a co-management vendor handle the billing process for both the physician and the home health agency?
A sophisticated co-management platform integrates direct, automated billing support.
- For the HHA: The system’s algorithm tracks daily cellular device transmissions and compiles monthly logs, automatically appending the correct flat-rate modifier (U2 through U9) to procedure code S9110 based on the exact transmission day count, and exporting a batched EDI 837I claim form to the clearinghouse.
- For the Physician: The system aggregates logged clinical minutes and interactive communications to generate an EDI 837P claim containing CPT 99091 (for Medicaid data interpretation) or 2026 Medicare codes (such as CPT 99445, 99454, and 99470), applying strict logic blocks to prevent overlapping or mutually exclusive billing errors before claims submission .
Q8: What features should we look for to ensure our co-managed program is compliant with OIG audit standards?
With the HHS OIG actively auditing remote care programs for billing fraud, your EMR and vendor must deliver “compliance by design”. The system must systematically generate an “OIG audit package” on demand, containing the signed physician’s order, the approved F00032 form, and documented patient consent . Furthermore, it must provide a complete, undeniable audit trail of clinical activity . This includes a daily physiologic data log displaying the exact days device transmissions were received (proving the 2-day or 16-day billing thresholds), detailed timestamped logs of clinical staff activity, and a clear, documented timeline of how abnormal, out-of-range biometric readings were clinically escalated and resolved .
Q9: How does this integrated telemonitoring framework shift the paradigm of care from expensive hospital stays to the patient’s home?
Integrated telemonitoring acts as a continuous digital safety net . In traditional home care, visiting nurses only evaluate a patient 1 to 3 times per week, leaving a dangerous “4-to-6 day gap” where clinical decline can go unnoticed and result in an emergency room visit. Cellular-enabled RPM devices allow the clinical team to capture daily, real-time physiologic data (such as rapid weight gain in a heart failure patient, indicating dangerous fluid retention) . This enables clinical staff or the HHA to intervene proactively – such as adjusting a medication dose long before a clinical crisis emerges . Evidence shows that combining continuous monitoring with care coordination reduces acute hospital admissions and length of stay by nearly 25% to 80%, saving millions in healthcare expenditures .
Q10: How much additional revenue can a physician practice realistically generate by stacking multiple digital care services?
By leveraging an HHA or a specialized vendor to do the operational heavy lifting, a physician practice can easily scale several complementary care programs simultaneously. Rather than just billing for a single remote monitoring code, the EMR platform allows providers to compliantly “stack” RPM with Chronic Care Management (CCM), Principal Care Management (PCM), Behavioral Health Integration (BHI), and Advanced Primary Care Management (APCM) for qualifying patients . While traditional, time-based CCM is historically administrative, the new APCM codes allow for capitated, monthly subcapitated G-codes (like G0558 at ~$110/month) based on patient complexity . By combining these stacked programs with the daily biometric logs of RPM, a single practice can compliantly generate over $300 to $400 or more per patient, per month in highly predictable, recurring revenue.